The Nursing Role
Within healthcare nurses have many roles. In a hospital setting nurses are responsible for caring for the sick and injured. They’re main job is to restore health and alleviate suffering of the patient. A nurse is “a person who has care of the sick, feeble or injured and has trained for the purpose” (Brooker 2008). In a hospital setting a nurse is the link between the doctor and patient. Generally the doctor will assess the patient and prescribe the treatment or course of action required e.g. deciding whether treatment is necessary, but it is the nurse that follows up the course of treatment giving pain medication and changing dressings as well as adhering to patients needs.
Nurses work in a variety of settings including: hospitals, surgeries, community, clinics, schools, nursing homes and hospices. This demonstrates the diversity of the nursing role as each setting requires specialist skills and knowledge within each nursing domain.
Nurses fulfilled a key role in the initial and ongoing assessment of client needs. Other contributions included providing technical and physical care, integrating therapy into their nursing practice and carrying on with therapy, building up relationships with the client and carer, co-ordinating care and discharge planning (Brooker 2008).
Nurses work in a variety of settings including: hospitals, surgeries, community, clinics, schools, nursing homes and hospices. This demonstrates the diversity of the nursing role as each setting requires specialist skills and knowledge within each nursing domain.
Nurses fulfilled a key role in the initial and ongoing assessment of client needs. Other contributions included providing technical and physical care, integrating therapy into their nursing practice and carrying on with therapy, building up relationships with the client and carer, co-ordinating care and discharge planning (Brooker 2008).
The Nursing Process
The Nursing process is suggested to be a cyclical process consisting of four elements which interconnect and can be revisited at any time; assessment, planning, implementation and evaluation (RCN 2004). Through implementing the nursing process it facilitates up-to-date documentation, evidence-based practice, accuracy and consistency. Therefore enhancing care delivery to patients, their families and friends. Also by using the nursing process inter-professional working is enhanced, professionals gain more job satisfaction and patient's care delivery is enhanced.
The above clip demonstrates the nursing process, and demonstrates its simplicity and how it can be implemented into everyday life.
Within the profession of nursing the assessment, management and evaluation of a patient is continually be monitored. Nurses uses this process to provide rationales for actions and ommissions. Nurses make referrals to the appropriate members of the MDT to meet the needs of each individual patient, utilising the skills and knowledge of other professionals .
Within nursing there is opportunities to specialise within a subject area such as pain, this suggests that adult nursing that is not specialised and relies on inter-professional collaboration in order to diagnose and prescribe for those with chronic pelvic pain. Nurses will continue to follow the nursing process to deliver effective care however, inter-professional working is key to the assessment and management of chronic pelvic pain.
Within the profession of nursing the assessment, management and evaluation of a patient is continually be monitored. Nurses uses this process to provide rationales for actions and ommissions. Nurses make referrals to the appropriate members of the MDT to meet the needs of each individual patient, utilising the skills and knowledge of other professionals .
Within nursing there is opportunities to specialise within a subject area such as pain, this suggests that adult nursing that is not specialised and relies on inter-professional collaboration in order to diagnose and prescribe for those with chronic pelvic pain. Nurses will continue to follow the nursing process to deliver effective care however, inter-professional working is key to the assessment and management of chronic pelvic pain.
Pain Assessment and Management
Dougherty and Lister (2011) say that the assessment of pain is an essential skill that nurses should posses; the assessment involves accumulating information from the patient. For example their experience/s of pain and how it impinges on their activities of daily living (ADL's) and their view of their quality of life. This enables nurses to gain an understanding of the patients’ individual experience of pain. Cummings and Bennett (2012) say that it is imperative that patients are treated as partners within their care process as they are the experts in how they feel through personal experience. It is the duty of the nurse to promote and facilitate joined-up care (Cummings and Bennett 2012).
Within primary care settings nurses carry out an holistic assessment with all their patients. Nurses have a duty to make referrals for their patients to ensure they receive the best treatment to meet their individual needs. If a patient was experiencing chronic pelvic pain the nurse would need to gain an understanding of how it is affecting the patient and their quality of life. Also if the patient is involved with the pain team and what medications they are currently taking.
Within primary care settings nurses carry out an holistic assessment with all their patients. Nurses have a duty to make referrals for their patients to ensure they receive the best treatment to meet their individual needs. If a patient was experiencing chronic pelvic pain the nurse would need to gain an understanding of how it is affecting the patient and their quality of life. Also if the patient is involved with the pain team and what medications they are currently taking.
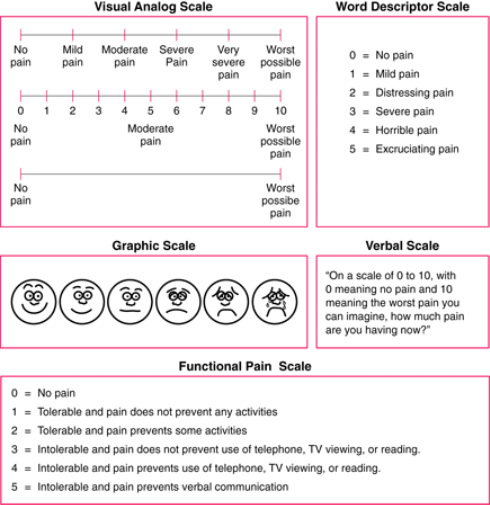
Below are some examples of measuring and assessing the pain. It is of the utmost importance that as nurses pain is assessed correctly. As pain is an individual experience the patient is the expert of their pain therefore, by using the six C's of nursing put forward by (Cummings and Bennett 2012) as professionals we can ensure that the patients needs are met to the best of our abilities, by practising inter-professional working, enabling the skills and knowledge required to meet the patients needs.
The variety of pain scales above, enable health care professionals to gain an understanding of the pain that the patient is experiencing. Each of the scale can be used within the health care environment for people of all ages and abilities, and across professions.
It is suggested by several authors within the literature that pain is said to be the fifth vital sign (Hinchy 2010; Casey 2011; Vijayaraghavan et al. 2012; Tousignant-Laflamme et al. 2012) however, there is evidence to suggest that pain whether chronic or not is under assessed and poorly managed within health care (Wells et al 2008). As nurses are at the forefront of the delivery of fundamental care needs to patient it is imperative that nurses have the skills and knowledge to assess and manage pain (Hichy 2010). Dougherty and Lister (2011) articulate that pain is not static therefore, pain assessment is an on-going process rather that a single event.
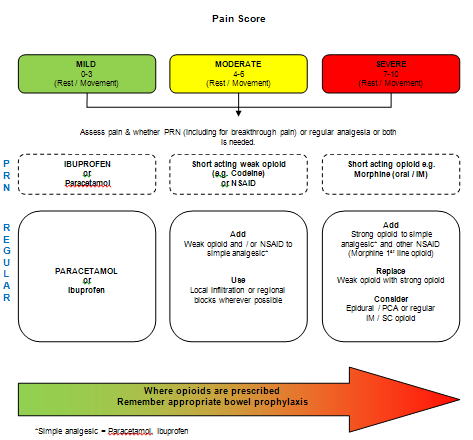
The World Health Organisation (WHO 1996) developed the analgesic pain ladder which is used within nursing practice to manage pain. It is suggested that people who experience chronic pain should receive analgesia around-the-clock in order for chronic pain to be controlled/ managed (Dougherty and Lister 2011).
The World Health Organisation (WHO 1996) developed the analgesic pain ladder which is used within nursing practice to manage pain. It is suggested that people who experience chronic pain should receive analgesia around-the-clock in order for chronic pain to be controlled/ managed (Dougherty and Lister 2011).
In order for nurses to manage a persons pain analgesia would need to be prescribed and would be given at the intervals that are recommended by the specialist pain team and/ or doctors. The pain relief provided would follow the WHO (1996) analgesic ladder to attempt to manage pain.
Nursing and Chronic Pelvic Pain.
It is suggested by Abercrombie and Learman (2012) that the assessment of chronic pelvic pain needs to be systematic and comprehensive in order to address the physiological and psychological causes. It is suggested by Abercrombie and Learman (2012) that there are specialist nurses in this field.
Prem et al (2011) suggests that their are inadequacies with the education of health care professionals for example nursing. Nurses are responsible for the management of pain as they hold the keys to the pharmacological therapies, nurses will only provide the medications that are prescribed by a doctor following the dose, frequency and route. If the nurse feels that there is a need for more pain relief he/ she will seek advice from a doctor or pain specialist.
Prem et al (2011) suggests that the assessment and management of chronic pain among nurses is affected by their attitudes and beliefs towards chronic pain. These attitudes and beliefs are moulded through education, personal experience, clinical experience and its setting.
Poor understand of the pathology of chronic pain causes nurses to poorly manage pain, and assess pain inadequately, it is suggested by Prem et al (2011) that the attitudes and beliefs of chronic pain held by some nurses cause them to be bias during assessment.
Prem et al (2011) suggests that their are inadequacies with the education of health care professionals for example nursing. Nurses are responsible for the management of pain as they hold the keys to the pharmacological therapies, nurses will only provide the medications that are prescribed by a doctor following the dose, frequency and route. If the nurse feels that there is a need for more pain relief he/ she will seek advice from a doctor or pain specialist.
Prem et al (2011) suggests that the assessment and management of chronic pain among nurses is affected by their attitudes and beliefs towards chronic pain. These attitudes and beliefs are moulded through education, personal experience, clinical experience and its setting.
Poor understand of the pathology of chronic pain causes nurses to poorly manage pain, and assess pain inadequately, it is suggested by Prem et al (2011) that the attitudes and beliefs of chronic pain held by some nurses cause them to be bias during assessment.